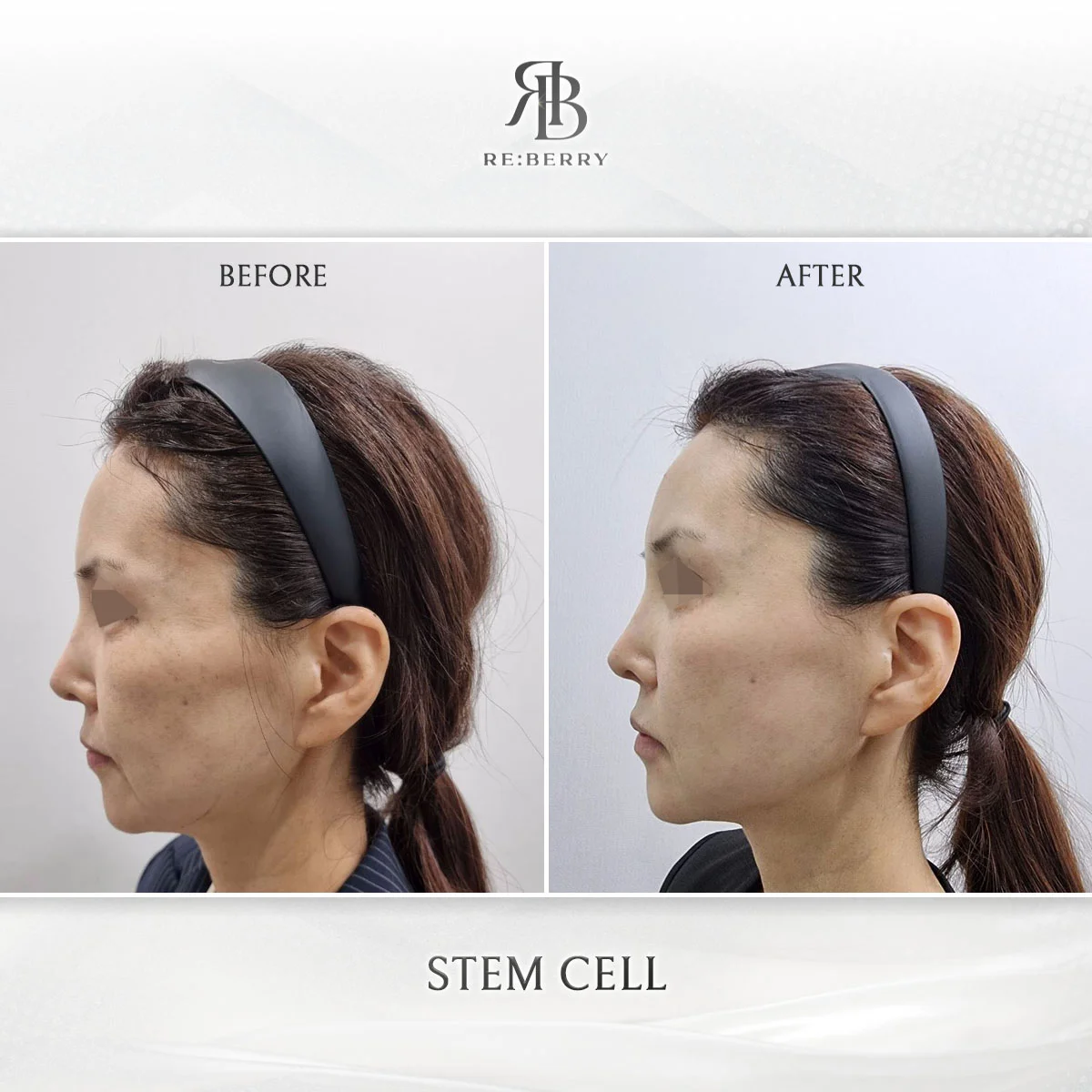
Who Benefits Most from Stem Cell Therapy
Stem cell therapy delivers the strongest results for patients experiencing early to moderate biological aging. The ideal candidate profile includes adults aged 30-65 who notice declining skin elasticity, loss of facial volume, increased fine lines, or overall skin texture deterioration. Because the treatment uses autologous blood (the patient's own biological material), it works across all 6 Fitzpatrick skin types without risk of allergic reaction, pigmentation complications, or immune rejection that can occur with synthetic treatments.
Age-Specific Candidacy Considerations
Patients aged 30-45 respond fastest to stem cell therapy because their baseline regenerative capacity remains relatively high, with fibroblast activity levels approximately 40-60% of peak function. Treatment at this age range produces visible improvement within 2-3 weeks and serves both rejuvenation and prevention purposes. Patients aged 45-55 benefit substantially but may require the multi-session Eternal Youth protocol (4 sessions) rather than a single-session approach to achieve equivalent collagen rebuilding. Patients over 55 are still strong candidates, though treatment plans typically incorporate complementary procedures like Revinas radiofrequency to amplify growth factor effects.
Skin Types and Conditions That Respond Well
The autologous nature of stem cell therapy eliminates the skin-type restrictions that apply to laser and light-based treatments. Darker skin tones (Fitzpatrick IV-VI) carry zero risk of post-inflammatory hyperpigmentation from the procedure itself, making it one of the safest regenerative options for patients of all ethnic backgrounds. Specific skin conditions that respond well include photoaged skin with sun damage, dehydrated skin lacking dermal volume, acne scarring with textural irregularity, and post-menopausal skin experiencing estrogen-related collagen decline.
Scalp applications suit candidates experiencing early-stage hair thinning (Norwood stages II-IV or Ludwig stages I-II). Growth factors stimulate dormant follicles and improve hair shaft thickness by increasing nutrient delivery to the dermal papilla. Patients with complete follicle loss (advanced alopecia) see limited benefit because the treatment requires viable follicle structures to regenerate.
Contraindications: Who Should Not Get Stem Cell Therapy
Approximately 8-12% of consultation patients present with conditions that temporarily or permanently contraindicate stem cell therapy. Absolute contraindications include active cancer or undergoing chemotherapy, blood clotting disorders (thrombocytopenia, hemophilia), active systemic infections, and pregnancy or breastfeeding. These conditions either compromise the quality of extracted growth factors or create unacceptable medical risks during the blood draw and processing stages.
Temporary Contraindications
Several conditions require treatment postponement rather than permanent exclusion. Patients taking blood-thinning medications (warfarin, aspirin, NSAIDs) must discontinue use 7-14 days before the procedure under physician guidance. Active skin infections or inflammation in the treatment area require resolution before injection. Patients with uncontrolled diabetes (HbA1c above 8.0%) need glycemic stabilization first, as elevated blood sugar impairs growth factor function and wound healing by 30-50%.
The Consultation and Screening Process
A proper candidacy assessment takes approximately 30 minutes and includes 3 components: medical history review, physical examination of the treatment area, and baseline blood work analysis. The medical history identifies contraindications including medication interactions, autoimmune conditions, and prior adverse reactions to any injectable treatment. Physical examination evaluates skin laxity grade, volume loss severity, and treatment area vascularity to determine optimal injection mapping.
Blood work analysis confirms platelet count (normal range 150,000-400,000 per microliter), rules out anemia that would compromise sample quality, and verifies clotting function. Patients with platelet counts below 100,000 per microliter produce insufficient growth factor concentration for therapeutic benefit. At RE:BERRY Gangnam, Aesthetic Medicine Specialist Yoon-Gon Ryu conducts candidacy assessments that match patients to the appropriate protocol tier based on their biological profile and treatment goals.
Preparing for Your Stem Cell Consultation
Preparation improves both consultation efficiency and treatment outcomes. Stop NSAIDs and aspirin 7 days before the consultation blood draw. Avoid alcohol for 48 hours prior, as it dehydrates blood plasma and reduces platelet quality. Arrive well-hydrated by drinking 2-3 liters of water in the 24 hours before your appointment. Bring a current medication list, recent blood work if available from the past 6 months, and documentation of any allergies or autoimmune diagnoses. This preparation allows the specialist to make an immediate candidacy determination rather than requiring a follow-up visit.